Ministry of Health & Family Welfare, Government of India has revised the Guidelines for Home Isolation of Mild/Asymptomatic Covid-19 cases. The guidelines are in supersession to the guidelines issued on the subject on 2nd July 2020.
As per the guidelines, the patients who are clinically assigned to be Mild/Asymptomatic are recommended for Home Isolation.
The Asymptomatic cases are laboratory-confirmed cases not experiencing any Symptoms and having Oxygen Saturation at room air of more than 94%. Clinically assigned Mild Cases are patients with Upper Respiratory Tract symptoms (&/or fever) without Shortness of Breath and having Oxygen Saturation at room air of more than 94%.
Patients eligible for Home Isolation
- The patient should be clinically assigned as a Mild/ Asymptomatic case by the treating Medical Officer.
- Such cases should have the requisite facility at their residence for Self-Isolation and for Quarantining the family contacts.
- A caregiver should be available to provide care on a 24×7 basis. A communication link between the Caregiver and Hospital is a prerequisite for the entire duration of isolation.
- Elderly patients aged more than 60 years and those with Co-morbid conditions such as Hypertension, Diabetes, Heart disease, Chronic Lung/Liver/ Kidney disease, Cerebro-Vascular disease, etc shall only be allowed isolation after proper evaluation by the treating medical officer.
- Patients suffering from immune-compromised status (HIV, Transplant recipients, Cancer therapy, etc.) are not recommended for Home Isolation and shall only be allowed after proper evaluation by the treating medical officer.
Instructions for the Home-Isolated Patient
Patient must isolate himself from other household members, stay in the identified room, and away from other people in the home, especially elderlies and those with co-morbid conditions like hypertension, cardiovascular disease, renal disease, etc.
The patient should be kept in a well-ventilated room with cross ventilation and windows should be kept open to allow fresh air to come in. Used Mask should be discarded only after disinfecting it with 1% Sodium Hypochlorite.
The patient should at all times use a triple-layer medical mask. Discard masks after 8 hours of use or earlier if they become wet or visibly soiled. In the event of caregiver entering the room, both caregiver and patient may consider using N95 mask.
The patient must take rest and drink a lot of fluids to maintain adequate hydration. Follow respiratory etiquette all the time. The patient shouldn’t share personal items with other people.
Frequent handwashing with soap and water for at least 40 seconds or clean with an Alcohol-based sanitizer. Ensure cleaning of surfaces in the room that are touched often (tabletops, doorknobs, handles, etc.) with 1% Sodium Hypochlorite solution.
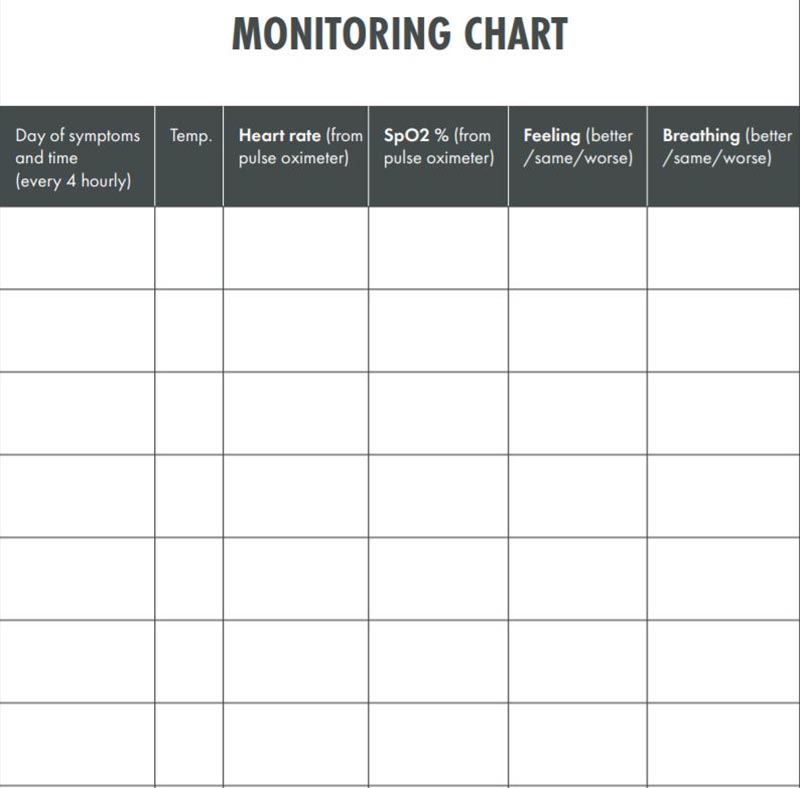
The patient will self-monitor his/her health with daily temperature monitoring and report promptly if any deterioration of symptoms as given below is noticed.
SpO2 reading:
- Normal: SpO2 should be 95% or above.
- If SpO2 is below 95 %, then the person should be immediately referred to the Supervisor/Medical Officer.
Thermal Screening reading:
- Fever: Any temperature of 100.4 F (38º Celsius) or greater is considered as Fever.
- If the temperature is higher, then the information should be immediately shared with the Supervisor/Medical Officer.
Instructions for Care-givers
The Caregiver should wear a Triple-layer Medical Mask. N95 mask may be considered when in the same room with the ill person. The front portion of the mask should not be touched or handled during use. He/she should avoid touching his Face, Nose, or Mouth.
If the Mask gets Wet or Dirty with Secretions, it must be changed immediately. Discard the mask after use and perform hand hygiene after disposal of the mask.
Hand Hygiene
- Hand hygiene must be ensured following contact with the ill person or his immediate environment.
- Hand hygiene should also be practiced before and after preparing food, before eating, after using the toilet, and whenever hands look dirty.
- Use soap and water for handwashing at least for 40 seconds. An alcohol-based hand rub can be used if hands are not visibly soiled.
- After using soap and water, the use of disposable paper towels to dry hands is desirable. If not available, use dedicated clean cloth towels and replace them when they become wet.
- Perform hand hygiene before and after removing gloves.
Exposure to Patient/Patient’s Environment
Avoid direct contact with the body fluids of the patient, particularly oral or respiratory secretions. Use disposable gloves while handling the patient.
Avoid exposure to potentially contaminated items in his immediate environment (e.g. avoid sharing cigarettes, eating utensils, dishes, drinks, used towels, or bed linen).
Food must be provided to the patient in his room. Utensils and dishes used by the patient should be cleaned with soap/detergent and water wearing gloves. The utensils and dishes may be re-used.
Clean hands after taking off gloves or handling used items. Use a triple-layer medical mask and disposable gloves while cleaning or handling surfaces, clothing, or linen used by the patient.
Biomedical Waste Disposal: Effective waste disposal shall be ensured to prevent the further spread of infection within the household. The waste (masks, disposable items, food packets, etc.) should be disposed of as per CPCB guidelines (available here).
Treatment for Patients with Mild/Asymptomatic cases in Home Isolation
Patients must be in communication with a treating physician and promptly report in case of any deterioration. Continue the medications for other co-morbid illnesses after consulting the treating physician. Patients to follow symptomatic management for fever, running nose, and cough, as warranted.
Patients may perform warm water gargles or take steam inhalation twice a day. If fever is not controlled with a maximum dose of Tab. Paracetamol 650mg four times a day, consult the treating doctor who may consider advising other drugs like a Non-Steroidal Anti-Inflammatory Drug.
The decision to administer Remdesivir or any other investigational therapy must be taken by a medical professional and administered only in a hospital setting. Do not attempt to procure or administer Remdesivir at home.
Systemic oral steroids are not indicated in mild disease. If symptoms persist beyond 7 days (persistent fever, worsening cough, etc.) consult the treating doctor for treatment with low-dose oral steroids.
In case of falling oxygen saturation or shortness of breath, the person should require hospital admission and seek immediate consultation from their treating physician/surveillance team.
When to seek Medical Attention? Patients / Caregivers will keep monitoring their health. Immediate medical attention must be sought if serious signs or symptoms develop. These could include
- Difficulty in breathing.
- Dip in Oxygen Saturation (SpO2 < 94% on room air).
- Persistent pain, Pressure in the Chest.
When to discontinue Home-Isolation? Patients under Home Isolation will stand discharged and end isolation after at least 10 days have passed from the onset of symptoms (or from the date of sampling for asymptomatic cases) and no fever for 3 days. There is no need for testing after the home isolation period is over.